Hot Topics at the 2016 Healthcare Design Expo & Conference
See predicted changes in healthcare identified at the conference...
See predicted changes in healthcare identified at the conference...
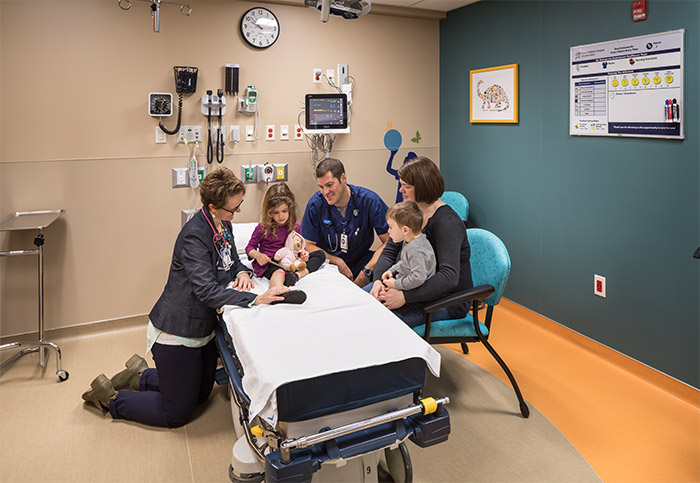
Design and health care professionals gathered this past November for the Healthcare Design Expo & Conference in Houston. Key trends focused on at the conference included preventative care, the role of technology, how changes in lab design are improving staff retention and efficiency, and the move toward a team approach to patient care.
With advancements in technology, new ways are emerging to help doctors and nurses operate in a more patient-friendly way without decreasing their focus on care. This could lead the healthcare industry to reduce cost and waste without sacrificing patient care.
An example of this is using smart phones as medical tools. Apps are being developed that allow doctors to use their smart phones as stethoscopes or to do biometric screenings. Doctors and patients also use smart phones to teleconference, saving patients a trip to the hospital or doctor’s office and saving time for both.
Other predicted changes in healthcare identified at the conference included:
Another trend discussed at the Healthcare Design Conference was the growth of patient-centered medical home care delivery model. These types of clinics focus on a team approach to patient care. One statistic given at the conference estimated that 75% of clinics nationwide are moving to this model.
In this type of clinic, patients are exposed only to the “onstage” areas (public areas such as lobbies, waiting rooms and corridors). Patients enter the exam rooms from the onstage areas by self-rooming or being escorted by staff. Within the layout of exam rooms is an “offstage” patient care and staff space, where all of the staff work; providers and nurses enter the exam rooms from the offstage area.
Some benefits of this structure:
The goal is to locate clinics in places convenient to patients, such as former stores. This way they are already on bus routes, with shopping and restaurants nearby and adequate parking. The more convenient the clinics are to people, the more people will use preventative care instead of putting off doctor visits until their problems worsen, increasing the cost of care.
The clinics offer self-rooming, where patients check in at kiosks. Many also include a respite or healing garden, where patients and staff can walk and get refreshed by nature.
There is a push to standardize the layouts of the exam rooms, with equipment and supplies always in the same spots. Providers can enter any room and know where everything is.
With 80% of all disease, illness and injury a result of people’s poor lifestyle choices, healthcare centers are turning their focus to prevention. The best place to start? With themselves, by fostering a “wellness culture” in the medical center.
Helping healthcare employees make healthier choices benefits the employees and patients because it has a mental effect on how they interact. If we take care of healthcare employees, they’ll be able to take better care of patients, leading to higher patient satisfaction.
Physical activity, nutrition and health education are the most cost-effective solutions. Therefore, healthcare facilities are offering benefits such as membership discounts to gyms and cooking and wellness classes. With the goal of attracting and retaining the brightest minds, hospital management teams are looking for designers to make staff spaces welcoming and energizing to keep employees happier at work:
Facilities are also looking at wellness outreach in their community. Medical fitness centers are being built that serve older, higher risk populations who may have never joined a fitness center before. Some differences between these and a regular fitness gym include medical supervision, an individual approach, and clinical integration – for example, cardio rehab or physical therapy.
In addition to bringing home baby, moms also want to bring home a positive, memorable experience from their birth center.
Whether it’s having a spa-like environment or making room for “crowd birthing,” birth center designs are catering to moms’ desire to be in control of their comfort and surroundings.
Examples of amenities being requested include:
Labs are becoming more inviting places designed to attract and retain staff and to be more efficient in their use of space and how resources are used.
With a number of lab projects currently underway at the University of Iowa Hospitals and Clinics (UIHC), Shive-Hattery is working with UIHC to incorporate the latest in lab design. A few of these design trends were discussed at the latest Healthcare Design Conference in Houston:
Since lab space and equipment are extremely costly, these three trends help with better utilization and reduced cost.
Another driving force in the design of labs is recruitment and retention. For example, designs are moving toward lower shelving and walls in between workspaces. This allows for more natural lighting and views to the exterior, making labs more visually appealing. It also enables people working long days at their desks to see each other, making work less lonely, thus leading to higher staff satisfaction.
With healthcare becoming so costly and competitive, the reality is design teams must plan their projects to be completed in the shortest possible time. Most projects involve rebuilding within an existing structure often sharing space with doctors, nurses and staff working 24/7. Therefore, projects need to be phased, and require a series of moves through a sequence of mini-renovations. Phasing of projects must also consider the impact of construction on patient safety and satisfaction. Construction dust has been determined to be one of the causes of hospital-acquired infections. Therefore, temporary air-tight and soundproof barriers must be erected around each construction zone, and each zone must have a negative air pressure to the surrounding occupied spaces. Without careful planning, multiple phase projects can significantly impact completion dates and cash flow.
In rebuilding the Pathology Core Lab at the UIHC, we created six zones to keep the lab operational. As we’d finish the remodel in one zone, we would reconfigure the space and move equipment to the next zone. Collaborating with staff not only kept everyone on the same page as construction progressed, but also helped drive the final design based on the new workflows resulting from the newly installed technology.